Can You Get Vitamin D from the Sun Without Harming Your Skin?
The science of safe sun exposure for vitamin D: how much you need, when to stop, and what sunscreen actually does to your levels.

Your skin produces vitamin D when UVB rays convert 7-dehydrocholesterol in the dermis to previtamin D3. In New Zealand, meaningful UVB exposure is available year-round in northern regions, but only for short windows before UV index reaches skin-damaging levels. A general guide: 10 to 15 minutes of midday sun on arms and legs in summer, longer in winter, then cover up or apply SPF.
New Zealand has the highest reported melanoma incidence rate in the world. It also has summer UV that peaks 40% higher than equivalent northern hemisphere latitudes, according to NIWA research. And yet vitamin D deficiency is a real and documented problem here, because most people get most of their vitamin D from the sun. These two facts sit in uncomfortable proximity. Getting the balance right genuinely matters, and the science has become clear enough to give practical guidance.
At Tōtika Health, our beekeepers work outdoors in the Bay of Islands sun year-round. Our apiaries sit in the Northland bush, where UV intensity is among the highest in the country. Sun safety is not a theoretical topic for us. This article sets out what the peer-reviewed evidence actually says, so you can make informed decisions about your own sun exposure.
How Your Skin Makes Vitamin D
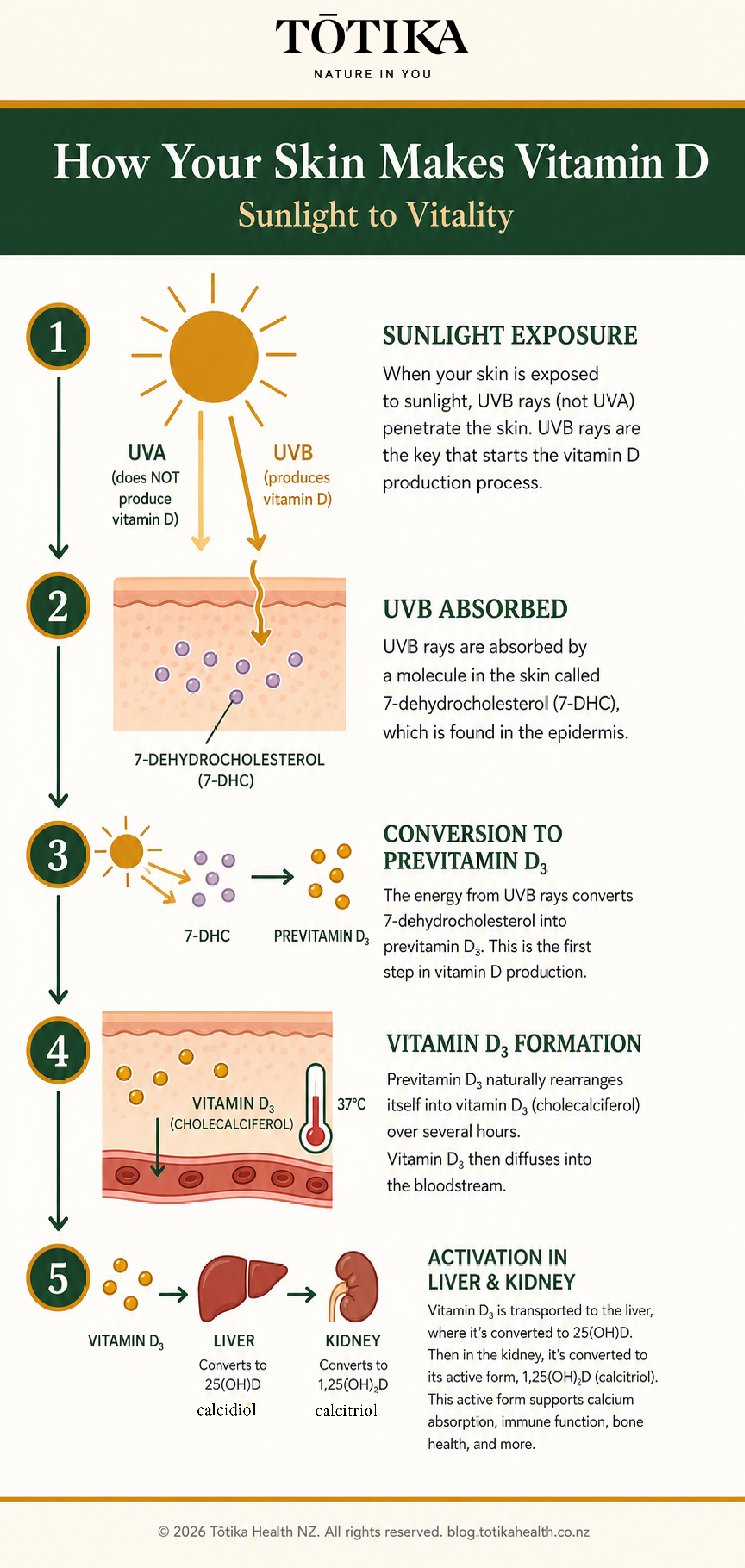
When sunlight reaches your skin, UVB radiation at wavelengths between 280 and 315 nanometres converts a cholesterol-derived compound called 7-dehydrocholesterol (found naturally in skin cells) into previtamin D3. Body heat at 37°C then converts previtamin D3 into vitamin D3, which travels via the bloodstream to the liver and kidneys, where it becomes the biologically active hormone form. The infographic above illustrates all five steps of this process.
Two things matter immediately. First, only UVB drives vitamin D synthesis. UVA, which makes up more than 95% of the UV radiation reaching Earth's surface, causes photoageing and immunosuppression but contributes nothing to vitamin D production. Second, UVB sufficient for vitamin D synthesis is only present when the UV Index (UVI) is 3 or above, meaning the sun must be reasonably high in the sky. In Northland at midday, this threshold is met year-round. In southern New Zealand during winter, it may not be.
The Problem: The Same Rays That Build Vitamin D Also Damage Skin
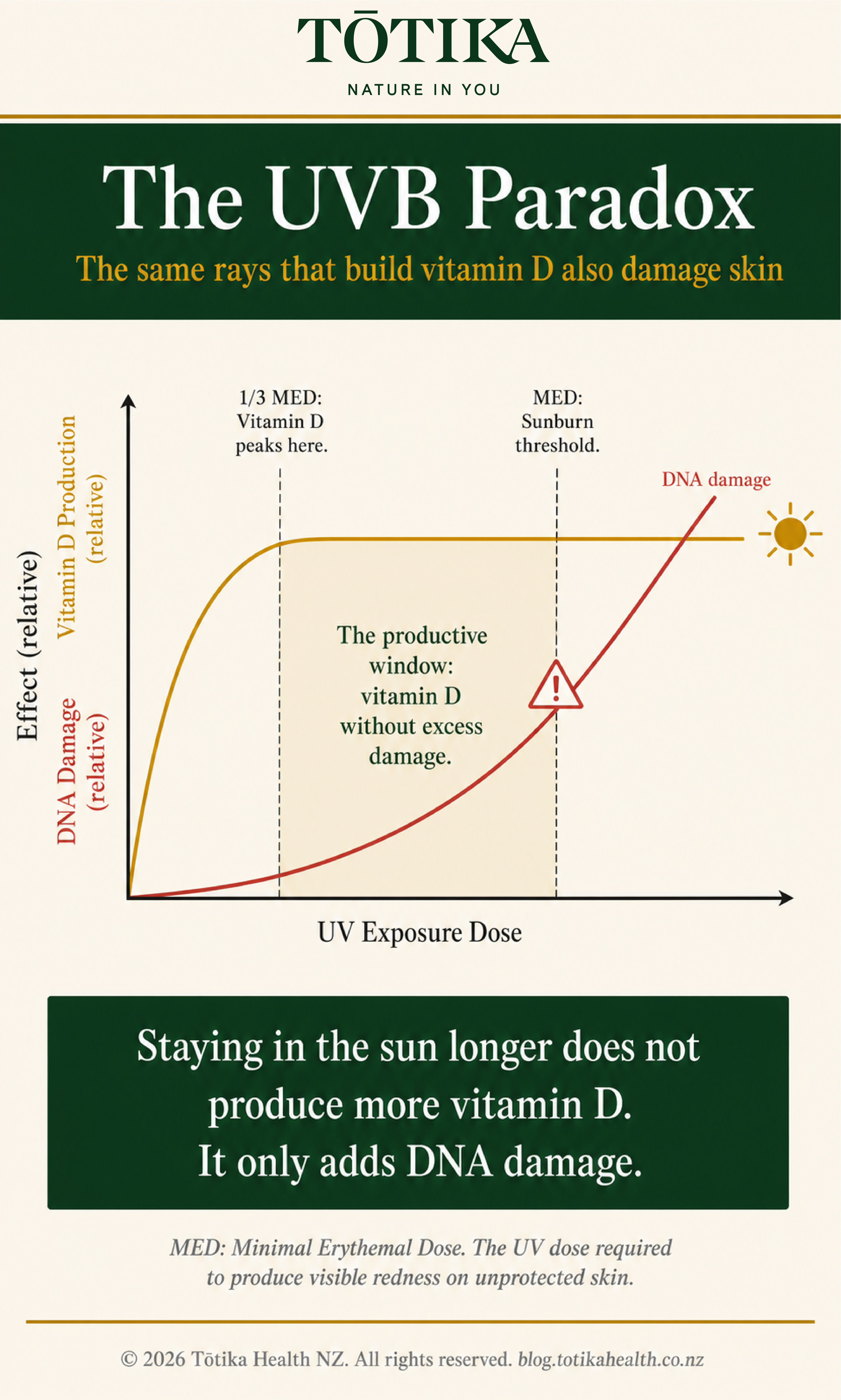
Here is the tension at the heart of this question. The same UVB wavelengths that trigger vitamin D synthesis also cause DNA damage in skin cells, specifically a type of molecular injury called cyclobutane pyrimidine dimers (CPDs). These are the lesions that initiate skin cancer when they accumulate and are not repaired.
A 2016 study by Felton and colleagues, published in the British Journal of Dermatology, tested this directly. Participants received repeated low-level summer UV exposures broadly comparable to brief regular outdoor activity. In fair-skinned individuals, vitamin D levels rose from deficient to adequate. Concurrently, measurable DNA damage appeared in skin cells immediately after exposure. The damage was low-level and largely repaired within 24 hours, but the central finding was unambiguous: vitamin D synthesis and skin DNA damage occur simultaneously, even at sub-sunburn doses.[1]
A 2018 study by Shih and colleagues extended this across all six Fitzpatrick skin types, from the fairest (type I) to the darkest (type VI). At fractional doses below the sunburn threshold, both vitamin D synthesis and epidermal DNA damage were detected across every skin type. The critical difference was location: in darker skin, melanin concentrated DNA damage in the superficial skin layers, protecting the deeper basal cells where most skin cancers originate. In fairer skin, damage was distributed evenly across the epidermis, including the basal layer, which explains the substantially higher skin cancer incidence in pale-skinned populations.[2]
As the diagram above shows, vitamin D synthesis does not increase proportionally with UV dose. It reaches its maximum at roughly one-third of the minimal erythemal dose (MED). Beyond that point, additional UV exposure produces no more vitamin D. It only increases cumulative DNA damage and sunburn risk. Staying out longer does not help. It only adds harm.
Can You Get Vitamin D Without Raising Skin Damage Risk?
The honest answer: yes, with important caveats that depend on your skin type, the UV Index on the day, and how much skin you expose.
The New Zealand Ministry of Health and Cancer Society's Consensus Statement on Vitamin D and Sun Exposure acknowledges this balance explicitly. For the general population, brief sun exposure is recommended for vitamin D synthesis, with emphasis on keeping it short and not intentionally sunbathing. When the UVI is 3, skin damage in fair-skinned individuals takes approximately an hour to become significant. Within that window, exposing the face, arms and legs for a few minutes is sufficient to produce meaningful vitamin D.[4]
NIWA atmospheric radiation research provides more specific guidance for New Zealand conditions. In summer, when Northland UV can reach UVI 13 or above, a few minutes of face and hands exposure around solar noon is sufficient for vitamin D. As the UVI rises, the margin between productive exposure and sunburn risk compresses significantly, so brevity matters more at the height of summer than at any other time of year.[5]
| UV Index | Skin Type I-II (fair, burns easily) | Skin Type III-IV (medium, tans gradually) | Skin Type V-VI (dark, rarely burns) |
|---|---|---|---|
| 3 (moderate) | 5 to 10 minutes, face and arms | 10 to 15 minutes | 20 to 30 minutes or more |
| 7 (high) | 2 to 5 minutes | 5 to 8 minutes | 10 to 15 minutes |
| 11+ (extreme) | Less than 2 minutes | 2 to 4 minutes | 5 to 8 minutes |
These are approximate exposure times for unprotected skin around solar noon. For most New Zealanders during summer, incidental daily sun exposure during a short outdoor walk is likely sufficient for vitamin D needs without any additional intentional exposure.
How to Strike the Balance: What the Research Recommends

The following guidance reflects the NZ Ministry of Health Consensus Statement, NIWA research, and the published peer-reviewed evidence. It is general information only. If you have personal risk factors for skin cancer or known concerns about your vitamin D status, please speak with your GP before changing your sun exposure habits.
Time your exposure around the UV Index
The Ministry of Health recommends outdoor activity in the early morning or late afternoon during summer, when the UVI is substantially lower than at midday. In early morning or after 3pm in Northland during summer, you have a more comfortable window for outdoor activity before sunburn risk becomes significant. Check the MetService UV forecast before outdoor time on high-sun days.
Expose enough skin area to matter
More skin area means more vitamin D synthesised, up to a biological maximum. Face, arms and legs uncovered is substantially more productive than face and hands alone. In winter, covering up is natural and necessary, which means vitamin D production from sunlight alone may be insufficient during the colder months. Dietary sources (oily fish, eggs, fortified foods) and supplementation can fill the gap; your GP can advise on whether supplementation is appropriate for you.
Stop before the sun damage accumulates
Once you have had your brief productive window (5 to 15 minutes depending on conditions and skin type), additional exposure adds no more vitamin D. Apply broad-spectrum sunscreen, put on a hat and shirt, or move into shade. This is not about avoiding sun entirely. It is about being precise rather than casual about the time you spend unprotected.
Know your UV Index before going outside
The MetService UV forecast provides daily UV Index data across New Zealand. At UVI 11 or above, which occurs on clear summer days in Northland, vitamin D exposure for a fair-skinned person takes less than two minutes. There is almost no window where staying outside unprotected longer becomes beneficial. This is the UV environment Northland residents live with from October through to March, and it demands respect.
Does Sunscreen Block Vitamin D Synthesis?

This is one of the most commonly asked questions, and the short answer is: probably not meaningfully, in the real world.
In laboratory conditions, sunscreen applied at full recommended thickness does significantly reduce UVB transmission and impairs vitamin D synthesis in artificial UV exposure testing. But real-world use tells a different story. In 2019, Passeron and colleagues published a comprehensive review by an international panel of 13 experts spanning endocrinology, dermatology, photobiology, epidemiology and biological anthropology. Their conclusion after reviewing all available evidence was that sunscreen use for daily and recreational photoprotection does not meaningfully compromise vitamin D synthesis under real-world conditions.[3]
The gap between theory and practice has a simple explanation: people rarely apply sunscreen at the full 2mg per square centimetre thickness used in controlled testing. Coverage is uneven. Many people accumulate some sun exposure before applying sunscreen, or before it takes full effect. Two Australian randomised controlled trials found no significant difference in vitamin D levels between consistent sunscreen users and non-users across an entire summer season.
The practical position: regular use of broad-spectrum SPF 30+ sunscreen for skin cancer prevention does not put your vitamin D status at meaningful risk. You should still use sunscreen whenever you are in high UV conditions beyond your brief productive window, and particularly during peak UV hours in summer.
The New Zealand Context: Why This Matters Here
New Zealand sits at a latitude range from approximately 35 to 47 degrees south, but the UV environment here is significantly more intense than northern hemisphere equivalents. NIWA measurements show that summer peak UV in New Zealand runs 40% higher than at corresponding latitudes in the northern hemisphere, due primarily to lower levels of stratospheric ozone over the southern hemisphere and lower aerosol pollution in the atmosphere.[5]
New Zealand also has the highest reported melanoma incidence rate in the world, and skin cancer is the most common cancer in New Zealand, with an estimated 50,000 or more new cases annually. A significant proportion of the New Zealand population has fair skin types (Fitzpatrick I and II) that burn easily and carry elevated skin cancer risk. The risk here is genuinely high, which is why the Ministry of Health and Cancer Society's guidance is so cautious, and rightly so.[4]
For most New Zealanders during summer, incidental daily exposure during ordinary outdoor activity, a walk to the car, time in the garden, a lunch break outside, is likely sufficient for vitamin D without any additional intentional sun time. The risk is not that people get too little sun. The risk is that casual, prolonged, unprotected exposure accumulates over years without people realising the damage is building.
Who Should Not Rely on Sun Exposure for Vitamin D
For some people, intentional sun exposure for vitamin D is not appropriate. These include people with a personal or family history of melanoma or non-melanoma skin cancer, organ transplant recipients (who carry substantially elevated skin cancer risk due to immunosuppression), those taking photosensitising medications, and people with diagnosed photosensitivity conditions. For all of these groups, dietary sources and supplementation after discussion with a GP are the preferred route.
Older adults generally synthesise vitamin D less efficiently because concentrations of 7-dehydrocholesterol in the skin decline with age, and the kidneys become less able to convert vitamin D to its fully active form after around 50 years of age. This contributes to the higher prevalence of vitamin D deficiency in older populations even in relatively sunny climates.
People with darker skin (Fitzpatrick types V and VI) require substantially longer sun exposure for equivalent vitamin D synthesis than fair-skinned individuals, due to melanin's protective attenuation of UVB. For darker-skinned New Zealanders who spend most of their time indoors, or who live in southern New Zealand during winter, maintaining adequate vitamin D from sunlight alone may not be possible without very extended outdoor time, and supplementation is worth discussing with a GP.
Supporting Your Skin After Sun Exposure
Even brief, sub-erythemal UV exposure generates mild oxidative stress and a low-level inflammatory response in the skin. The skin barrier is subtly compromised after outdoor time in high-UV conditions, and the skin requires recovery time and support.
Tōtika Health's bioactive skincare range, formulated by Sara Samavati using certified mānuka honey bioactives and propolis extract, is designed to support skin barrier function and maintain hydration after exposure to environmental stressors, including UV. Building a simple post-outdoor skincare routine around barrier-supporting, bioactive moisturisation is a straightforward habit that complements sensible sun management.
Explore Tōtika's bioactive skincare range.
Frequently Asked Questions
Can I get vitamin D through a window?
Does sunscreen stop me making vitamin D?
How long do I need in the sun to get enough vitamin D?
What time of day is best for vitamin D from the sun?
Can I get enough vitamin D in a New Zealand winter?
Does cloud cover affect vitamin D synthesis?
If I have darker skin, do I need more sun exposure for vitamin D?
References
- Felton SJ, Cooke MS, Kift R, Berry JL, Webb AR, Lam PMW, de Gruijl FR, Vail A, Rhodes LE. Concurrent beneficial (vitamin D production) and hazardous (cutaneous DNA damage) impact of repeated low-level summer sunlight exposures. Br J Dermatol. 2016;175(6):1320-1328. doi:10.1111/bjd.14863. PMID: 27411377
- Shih BB, Farrar MD, Cooke MS, Osman J, Langton AK, Kift R, Webb AR, Berry JL, Watson REB, Vail A, de Gruijl FR, Rhodes LE. Fractional sunburn threshold UVR doses generate equivalent vitamin D and DNA damage in skin types I-VI but with epidermal DNA damage gradient correlated to skin darkness. J Invest Dermatol. 2018;138(10):2112-2121. doi:10.1016/j.jid.2018.04.015. PMC6158343.
- Passeron T, Bouillon R, Callender V et al. Sunscreen photoprotection and vitamin D status. Br J Dermatol. 2019;181(5):916-931. doi:10.1111/bjd.17992. PMC6899926.
- Ministry of Health and Cancer Society of New Zealand. Consensus Statement on Vitamin D and Sun Exposure in New Zealand. Wellington: Ministry of Health; 2012. Available at: health.govt.nz
- McKenzie R, NIWA. Balancing risks and benefits of UV radiation. Water and Atmosphere (NIWA). 2009;17(1). Available at: niwa.co.nz
- Holick MF. Sunlight and vitamin D: a global perspective for health. Dermatoendocrinol. 2013;5(1):51-108. doi:10.4161/derm.24494. PMC3897598.





